Sunstone Spotlight
Here we share with you all things related to the diagnosis, treatment, and care of our beloved pets. Check back often as there is always something new to learn. If there is a particular topic you are curious about, let us know and we may just include the answer in a future blog post.

Pet Safety, Tests and Procedures
Chronic diarrhea in dogs can be concerning pet owners. While it might seem like a minor inconvenience at first, ongoing diarrhea often signals underlying health problems. If your...

Pet Safety, Tests and Procedures
Coughing in dogs isn’t just a funny noise; it can signal underlying health issues. Coughing is a common issue that can happen for various reasons. Understanding why dogs...

Pet Safety, Tests and Procedures
At Sunstone Veterinary Specialists, we know how concerning it can be when your pet experiences health issues like diarrhea. As a veterinary internal medicine specialist, I frequently see cases...
Pet Safety
Introduction Let’s talk about your pet’s poop! While it might seem awkward, your pet’s stool can be one of the best indicators of their overall health. That’s where...

Pet Safety, Tests and Procedures
How Do We Measure a Pet’s Quality of Life? Hello there, When it comes to end-of-life decisions for pets, one of the most important things we must consider...

Emerging News, Pet Safety, Sunstone Updates, Tests and Procedures
Scheduling your pet’s Internal Medicine Consultation at Sunstone Veterinary Specialists is an important step in ensuring they receive expert care for complex medical issues. Our goal is to...
Sunstone Updates, Tests and Procedures
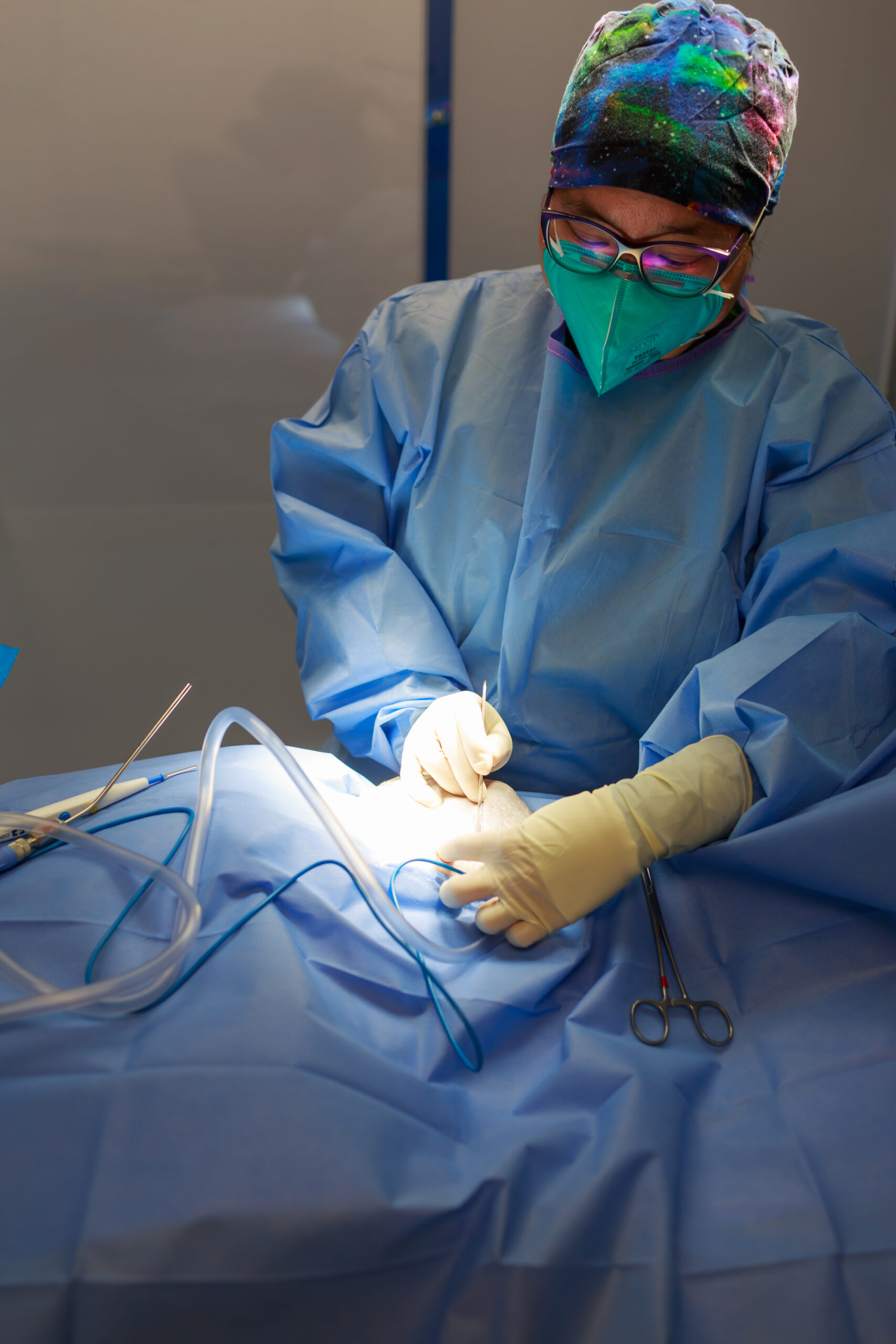
CCL Tear in Dogs: Causes, Symptoms, and Treatment A CCL tear in dogs is one of the most common causes of hind leg limping. The Cranial Cruciate Ligament...
Sunstone Updates, Tests and Procedures
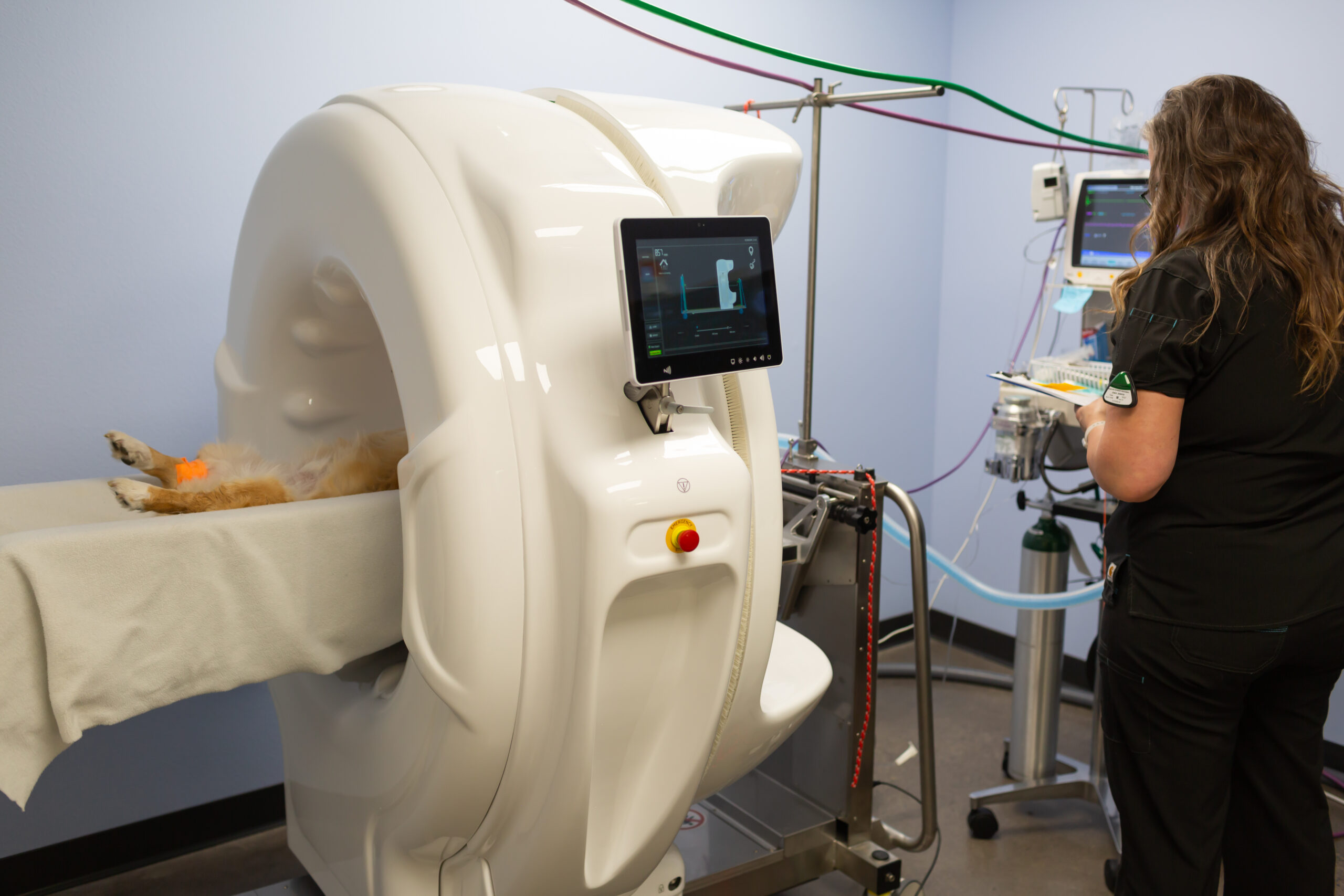
Introducing Advanced Imaging for Pets: What Makes HDVI Special? At Sunstone Veterinary Specialists, we are thrilled to introduce a groundbreaking imaging technology to our community: HDVI for pets....

Sunstone Updates, Tests and Procedures
In the last installment of our blog, we introduced you to one of our favorite diagnostic tools- endoscopy! We went over the basics and talked about gastrointestinal endoscopy,...

Sunstone Updates, Tests and Procedures
Welcome to the next installment of the Sunstone Vets Blog! This week, we will be talking about one of our favorite, minimally invasive diagnostic tools…..endoscopy! Endoscopy is a...
Tests and Procedures
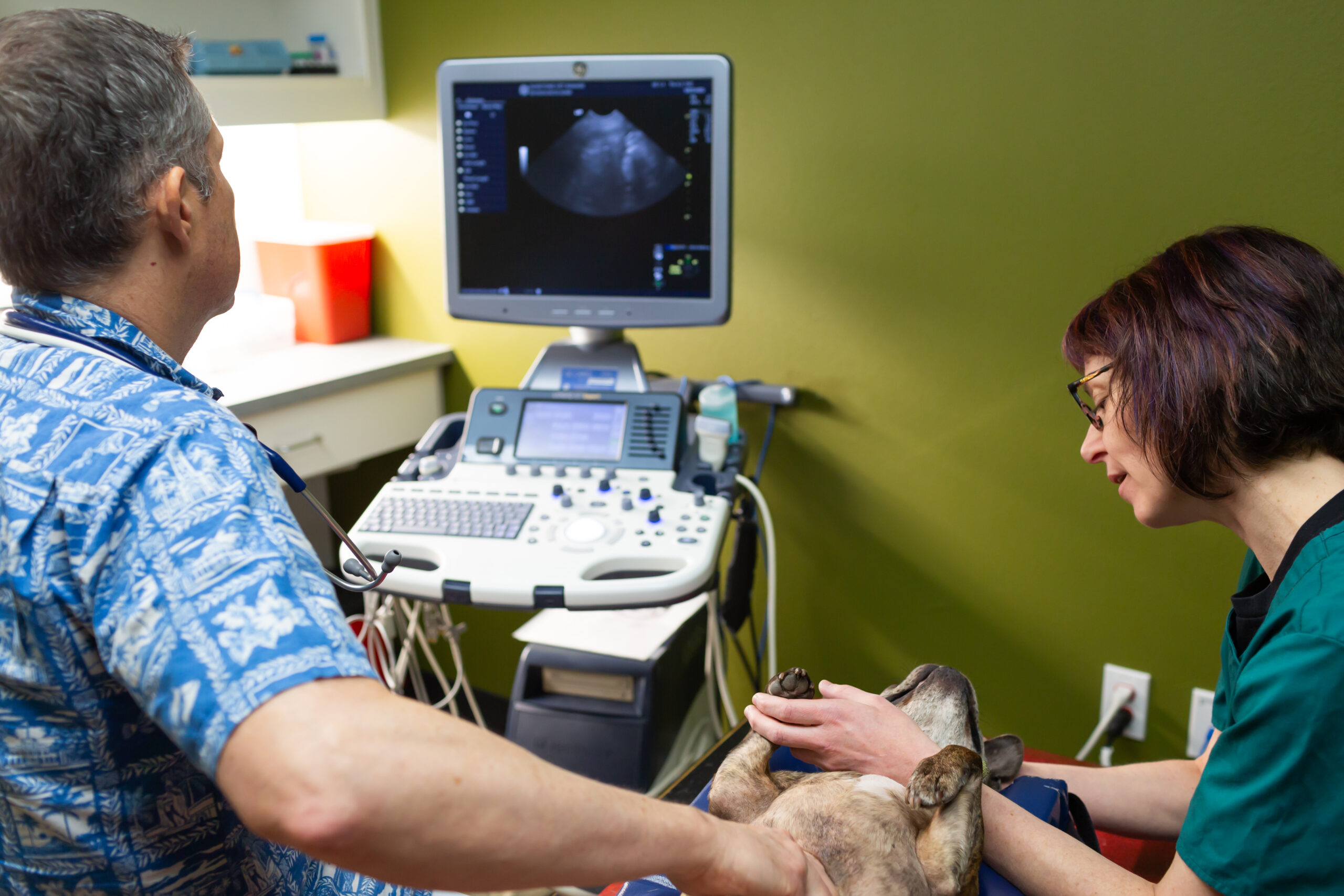
If you are reading this blog, your pet has likely been advised to have an abdominal ultrasound for some type of health issue they are having. So,...